Dr. David Brady, Guest
Thyroid Nation
An Excerpt from the Amazon Bestselling Book The Fibro Fix
The thyroid gland consists of two lobes, one on either side of the trachea (windpipe) in the lower neck. A portion connecting the two lobes, called the isthmus, gives the entire gland an H-shaped appearance. The thyroid gland is responsible for synthesizing several hormones that have vast effects on overall body metabolism. The thyroid is unique among the endocrine glands in that large amounts of hormone are created and stored in the thyroid itself and then released very slowly. Iodine ingested from food and water is concentrated in the thyroid gland, where it combines with the amino acid tyrosine to create the thyroid hormones triiodothyronine (T3) and thyroxine (T4). The numbers 3 and 4 identify the number of iodine units in the hormone’s structure. Generally speaking, lower levels of thyroid hormone will slow overall metabolism and energy, while higher levels will increase overall metabolism and energy. Thyroid-stimulating hormone (TSH), produced in the pituitary gland in the brain, influences all reactions controlling the formation of T3 and T4 (See Figure 1).
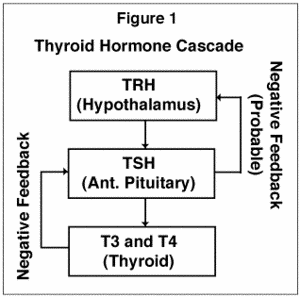 Figure 1: Thyroid hormone cascade.
Figure 1: Thyroid hormone cascade.
Having low thyroid function without actually having thyroid disease is very common, especially as we get older. Diminished thyroid function after age 40 occurs in about a quarter of the population. Because it’s not an overt illness, this type of low thyroid is sometimes called subtle or subclinical hypothyroidism. The symptoms are too minor to be declared an illness or disease according to standard medical measures. Yet, at the same time, they are too troublesome to allow you to feel really good. Symptoms of subtle functional hypothyroidism include:
- Fatigue
- Gradual weight gain that is hard to lose
- Muscle and joint achiness
- Dry skin
- Dry thinning hair
- Thinning of the outer third of your eyebrows
- Facial puffiness
- Mental sluggishness
- Cold hands and feet; a general feeling of being cold
You can see why many with sub-optimal thyroid function can be easily misdiagnosed as having fibromyalgia.
In addition to these symptoms, people with a clinical hypothyroid condition may experience:
- Extreme fatigue/low energy
- Weight gain
- Difficulty with concentration
- Inability to tolerate exercise
- Cold all the time
- Constipation
- Chronic infections
- Frequent postnasal drip
- Weakness
- Muscle cramps/aches
- Joint pain
- Numbness/tingling
- Hard time remembering things
- Carpal tunnel syndrome
- High blood sugar
- High blood fats (cholesterol)
- Swollen look to face
Thyroid function laboratory tests should be routinely performed in patients who present with complaints of widespread pain and fatigue in order to rule out significant or overt hypothyroidism as the cause of these symptoms. These tests should include thyroperoxidase antibodies (TPA) and thyroglobulin antibodies (TGA) tests to screen for cases of autoimmune thyroid conditions such as Grave’s disease and Hashimoto’s thyroiditis. Even when standard lab values are within the normal ranges, subtle variations of thyroid dysfunction should be considered.
Understanding T3 and T4
Many cases of hypothyroidism will respond well to the use of common hormone replacement medications, such as Synthroid, Levothroid, or Levoxyl. However, these medications contain only a synthetic version of the hormone thyroxine (T4). The problem here is that to be useful, T4 (the comparatively inactive “storage” hormone) must be converted to T3 (the “active” hormone) and some people are unable to do so very well. Instead, they produce too little of the active T3 and too much of the mainly inactive form of the T3 hormone, known as reverse T3 or “rT3.” (See Figure 2). This condition is sometimes referred to as euthyroid sick syndrome, low T3 syndrome, or thyroid hormone peripheral conversion disorder. In these situations, people often do not feel relief of their symptoms when placed on synthetic T4 alone.
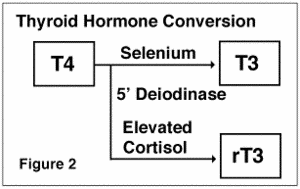 Figure 2: Thyroid hormone conversion.
Figure 2: Thyroid hormone conversion.
These types of thyroid dysfunction are more subtle than the kinds of problems conventional family doctors, and even most endocrinologists screen for. One possible reason for these conversion problems may be elevations in the level of the adrenal hormone cortisol due to acute or long-term stress. Cortisol is known to negatively affect the enzyme that converts T4 to active T3, called 5’-deiodinase. The use of combinations of T4 and T3 (for example, the porcine-derived Armour Thyroid and NatureThroid, or the combination of the synthetic medications Synthroid and Cytomel) are gaining popularity with many physicians attempting to help people with this issue. However, too often conventional doctors will tell people that their thyroid is just fine. Often that is just not so.
In my view, it would be better for doctors to pay close attention to all your clinical symptoms, to measure your core temperature, and to use comprehensive thyroid laboratory testing to gain a complete and accurate picture of your thyroid function. If the resulting laboratory results show that you are in the lower part of the normal range for both the total and free forms of the T3 and T4 hormones—or if your TSH results are in the upper part of the normal range, a functional medicine physician will typically consider a trial of comprehensive thyroid hormone treatment if you also have many clinical symptoms of low thyroid function.
Thyroid Hormone Markers
Here’s what you’ll learn from a thyroid panel. A high TSH indicates an underactive thyroid. In addition, the panel also separately tests T3 and T4 levels. T4 and T3 each exist in two forms: either bound to proteins in the blood, where they are kept in reserve for later use, or “free” T3 and T4 (known as FT3 and FT4) and immediately available to enter body tissues wherever needed to upregulate your metabolism. High levels of T4 and/or T3 suggest hyperthyroidism, while low levels of either T4 or T3 suggests hypothyroidism. In some cases of hyperthyroidism, FT4 is normal yet FT3 is elevated. Attention must be paid to the level of the free hormones, particularly free T3, for an accurate picture of what is happening metabolically from a functional perspective. Even a free T3 in the lower level of the “normal” range can indicate sub-optimal thyroid function if clinical symptoms and complaints typical of hypothyroidism are also present. However, if your doctor does not test this, you will simply never know.
Subclinical hypothyroidism can also be due to an autoimmune disorder known as Hashimoto’s disease, in which the immune system attacks the thyroid gland. Hashimoto’s can initially cause hyperthyroidism, but will eventually result in exhaustion of the thyroid due to tissue damage to the gland and an inability to produce an adequate amount of thyroid hormone. Functional hypothyroidism may also occur when, over a long period of time, the body has sent out too many false alarms to initiate the fight-or-flight response due to stress. These false alarms arouse the adrenals and thyroid to action. This is why it’s important to evaluate the status and functioning of the adrenal glands along with the thyroid.
In my experience, undiagnosed thyroid issues are one of the prime reasons for complaints of fatigue, achiness, and cognitive dysfunction—and the eventual misdiagnosis of pain and fatigue conditions like fibromyalgia (FM)—particularly in women.
Donna’s Story
After complaints of general pain and achiness, fatigue, insomnia, un-refreshed sleep, and mild depression, Donna was diagnosed with FM by her family doctor. He put her on an SSNRI antidepressant called venlafaxine (Effexor) and zolpidem tartrate (Ambien), a gamma-aminobutyric acid (GABA) receptor agonist, to help her sleep. For people with classic FM, these medications can be helpful, but all they seemed to do for Donna was to make her feel more groggy and spacey, without any real improvement in her symptoms. Although she didn’t realize it at the time, this was one important clue that Donna did not have classic FM. Hoping that there might be another road to recovery from her nexus of symptoms, Donna attended a teleseminar in which I presented. She decided to make an appointment and came to my office seeking alternative approaches.
I began by ordering a number of tests that show how well various bodily functions are working. These included:
- Blood chemistry: This test is used to assess the overall function of the major organs and systems of the body, but is designed to find overt disease, not optimal “function.”
- Complete blood count (CBC): The CBC is used to determine an individual’s general health by detecting the presence of anemia, infection, inflammation, bleeding disorders, and many other conditions such as blood-based cancers like leukemia and lymphomas.
- Iron studies: Three tests (serum iron, serum ferritin, and percent iron saturation) that together evaluate levels of iron in the bloodstream and various tissues. Low levels of iron are associated with a specific form of anemia known as microcytic anemia, which can result in an inability of the red blood cells to efficiently carry oxygen. This can result in metabolic dysfunctions, especially in the production of energy, making you fatigued and leaving you with achy muscles.
- Erythrocyte sedimentation rate (ESR): a simple, inexpensive, test that is used to detect systemic, or body-wide, inflammation. ESR is said to be “nonspecific” because, while an elevated result indicates inflammation, the test does not tell the practitioner where the inflammation is or what is causing it.
- C—reactive protein (CRP): Within a few hours of a tissue injury, infection, or other source of inflammation, the liver releases CRP into the blood. This test for CRP can be used together with symptoms and other tests to help determine if an acute or chronic inflammatory condition exists.
- Thyroid Panel: The thyroid panel tests for thyroid-stimulating hormone (TSH), various forms of the thyroxine (T4) and triiodothyronine (T3) hormones, and thyroid-related autoantibodies to screen for autoimmune diseases of the thyroid like Hashimoto’s and Graves thyroiditis.
Donna’s lab reports showed normal blood chemistry, CBC, and iron studies, and she was negative for certain key inflammatory markers (i.e., the ESR and CRP tests). Her thyroid panel was also technically normal, but on closer examination of the hormone levels, it became clear that there were certain imbalances, leading to sub-optimal function.
I saw that the total and free T3 levels were at the very bottom of the normal range, while the total and free T4 levels were also sub-optimal, though better than the T3 levels. Her TSH was still in the normal range but in the very high part of the range. In sum, the amount of active thyroid hormone she was getting was low, and her body was asking for more.
Another test that I frequently order for my patients is organic acid testing (OAT). This can often reveal issues in the biochemistry of energy production, which accompany low or suboptimal thyroid drive. When Donna’s test results came in, they revealed some inefficiencies in energy production. They also showed that Donna was not detoxifying chemicals and hormones that needed to be cleared from her body effectively. The serotonin metabolite (5-HIAA) was also low, but the stress hormone (catecholamine) metabolites were normal, which indicated that she may have been a bit deficient in her ability to manufacture on optimal amount of the important neurotransmitter hormone serotonin, but that she was not presenting with the stress pattern typical of classic FM, which often results in anxiety and insomnia in true classic FM patients.
By giving me an inside picture of what was going on in her body, these tests taken all together revealed to me that Donna mainly had functional hypothyroidism due to suboptimal thyroid hormone production, as well as poor thyroid hormone conversion of T4 to T3. She also had some issues with her unique biochemistry and metabolism which needed some tweaking, including supporting a more robust ability to produce energy in the cells and to detoxify waste products that need to leave the body, and raising her ability to produce serotonin.
Donna’s Treatment Plan
 At my urging, Donna went on the 21-day foundational plan outlined in the book The Fibro Fix, with its anti-inflammatory and non-allergenic fresh food diet. She began taking CoQ10, L-carnitine, D-ribose, and B-complex vitamins (for energy and mitochondrial metabolism support). For thyroid support, she began taking NatureThroid, which supplies both the T3 and T4 hormones; a supplement containing selenium, N-acetyl-tyrosine, and iodine to support thyroid hormone production and conversion, and a bit of 5-HTP for better serotonin production.
At my urging, Donna went on the 21-day foundational plan outlined in the book The Fibro Fix, with its anti-inflammatory and non-allergenic fresh food diet. She began taking CoQ10, L-carnitine, D-ribose, and B-complex vitamins (for energy and mitochondrial metabolism support). For thyroid support, she began taking NatureThroid, which supplies both the T3 and T4 hormones; a supplement containing selenium, N-acetyl-tyrosine, and iodine to support thyroid hormone production and conversion, and a bit of 5-HTP for better serotonin production.
Follow-up thyroid lab tests performed 4 weeks later guided me in adjusting the dosage to keep Donna in the upper 50 percent of all thyroid hormone-fraction ranges, but never above the normal range. For her occasional sleep issues, she began taking 3 mg of sustained-release melatonin just prior to bedtime.
After thirty days, Donna showed a 75 percent improvement in all symptoms (fatigue, achiness, insomnia, and non-refreshing sleep). After sixty days, her symptoms disappeared. A six-month follow-up showed that her condition had not returned.
Getting the thyroid working optimally is essential. If it’s not working well almost nothing else will. It’s something I pay as much attention to in my practice as anything else with chronically ill patients. Therefore, if you are not currently working with a doctor who is trained in integrative medicine, and even more specifically in functional medicine, and you think you may have an issue with your thyroid based on what you have read here, please find a physician who will give you a comprehensive thyroid function evaluation. If you can’t come to see me in my practice in Connecticut, you may want to consult the practitioner search tool through the Institute for Functional Medicine at https://www.functionalmedicine.org/ for some options on how to find a provider trained in the functional medicine approach.
About the Author
 Dr. David M. Brady is a leading naturopathic medical doctor at Whole Body Medicine in Fairfield, Connecticut. He is the vice president for Health Sciences and the director of the Human Nutrition Institute at the University of Bridgeport and the chief medical officer of Designs for Health, Inc., and Diagnostic Solutions Laboratory, LLC. Dr. Brady is a highly sought after presenter and prolific author of medical papers and research articles on autoimmune conditions, functional gastrointestinal problems, thyroid issues, as well as a dedicated champion and advocate for patients suffering with a fibromyalgia diagnosis. To learn more about functional hypothyroid disorders, please visit the “Media” tab at DrDavidBrady.com. To learn more about Dr. Brady’s approach to thyroid disorders, as well as pain & fatigue conditions like fibromyalgia, and more about his new book, The Fibro Fix, please visit FibroFix.com. Be sure to follow him on Facebook, Twitter, and Instagram.
Dr. David M. Brady is a leading naturopathic medical doctor at Whole Body Medicine in Fairfield, Connecticut. He is the vice president for Health Sciences and the director of the Human Nutrition Institute at the University of Bridgeport and the chief medical officer of Designs for Health, Inc., and Diagnostic Solutions Laboratory, LLC. Dr. Brady is a highly sought after presenter and prolific author of medical papers and research articles on autoimmune conditions, functional gastrointestinal problems, thyroid issues, as well as a dedicated champion and advocate for patients suffering with a fibromyalgia diagnosis. To learn more about functional hypothyroid disorders, please visit the “Media” tab at DrDavidBrady.com. To learn more about Dr. Brady’s approach to thyroid disorders, as well as pain & fatigue conditions like fibromyalgia, and more about his new book, The Fibro Fix, please visit FibroFix.com. Be sure to follow him on Facebook, Twitter, and Instagram.
PLEASE take a moment to ‘Like’ us on Facebook and follow us on Twitter and Pinterest. You can also listen to Danna and Tiffany on Thyroid Nation RADIO.
Questions or anything to add about thyroid hormones and subtle hypothyroidism? We want your thoughts, please. You might just help someone else in need.
Sources:
- Neeck G, Riedel W, Schmidt KL. Neuropathy, myopathy and destructive arthropathy in primary hypothyroidism. J Rheumatol 1990;17:1697-700.
- Khaleeli A, Griffith DG, Edwards RH. The clinical presentation of hypothyroid myopathy and its relationship to abnormalities in structure and function of skeletal muscle. Clin Endocrinol 1983;19:365-76.